Knee Inside Pain: The Tennis Elbow of the Knee
I was curious to see what patients were being shown about pain at the inside of the knee so I performed a web search. The term, “knee inside pain” popped up so I clicked on it. What was interesting was that almost all of the information about pain at the inside of the knee was about the meniscus and knee arthritis and not about the pes anserine area. The pes anserine is a strange name for what amounts to the tennis elbow of the knee-an area where many important muscles/tendons attach and that’s frequently associated with pain. Based on our experience, this is one of the most under diagnosed problems of the knee and is frequently the cause of inside of knee pain often blamed on other problems in the cartilage and meniscus. Patients with pes anserine tendon problems (sometimes called bursitis or tendopathy) have pain on the inside of the knee, just below the joint. If you feel around on your knee right now, you can likely make out where the two bones meet (the joint line) on the indie. The pes anserine area is just below that and in the front and is located where the tibia bone starts to slope downward. To illustrate how we think about the complex biomechanical causes of knee pain, I’ll illustrate a patient I saw yesterday in clinic. This is a middle aged gentleman who is very active and first injured his knee in high school during an football tackle to the outside of his knee. He was told he injured his ACL and this ultimately lead to several surgeries, culminating in one where they chopped out pieces of his lateral meniscus. He was first seen by our clinic about two years ago and while he made solid incremental improvements with Regenexx-C, at his last visit I knew we were missing something else. Our prior focus had been on his cartilage lesions in the knee, but his examination at the last visit had shown that most of his remaining tenderness was over the pes anserine area. So in addition to treating his cartilage, I injected some of the stem cells at that location. Seeing him in the office this past week, he relayed that his knee took a huge leap in improvement from the last treatment. This caused me to take another look at the other biomechanical aspects of his knee. On ultrasound imaging combined with physical exam, his MCL was also lax. For the first time all of the pieces of the puzzle fell in place on this patient.
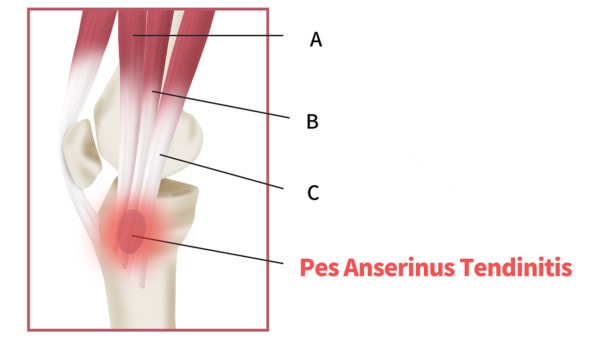
Chu KyungMin/Shutterstock
The illustration above is of a very simple knee joint drawn by me for illustration purposes. Note that in the left picture you see the two bones (in this case the blue rectangles) coming together to form the knee joint with the grey meniscus tissue drawn as triangles. The MCL ligament is on the left of the knee joint (inside) and is drawn in red, while the LCL ligament is drawn in green and is on the right of the joint (outside). These ligaments act as the duct tape that hold the knee together in a lateral direction. When this patient was hit in high school, while the medical team focused on the more injured ACL, they missed that his MCL was also damaged and loose. This is a very common missed finding, as we’ve seen many patients walking around with lax MCL ligaments that have gone undiagnosed. Note that in the picture on the left, the Sartorius, Gracilis, and Semitendinosis thigh muscles all attach at a common point, the pes anserine. When this patient was active with his lax MCL ligament, his knee would collapse inward slightly because the stretched MCL ligament allowed that movement (red ligament). The only muscles in the correct spot to help support the inside of the knee as it collapses inward would be the pes anserine muscles. Hence as the knee collapsed in this direction, the attachment of the pes would be overloaded and become painful as these muscles weren’t designed to take the place of a bad ligament. More importantly, the outside meniscus would become pinched (the red star on on the grey meniscus). This is why his lateral meniscus eventually failed and he needed a surgery there for a torn meniscus. Regrettably, chopping out the torn pieces did little to fix the real problem (the lax MCL ligament), so his pain continued. In summary, this patient had chronic lateral meniscus trauma because his MCL ligament was lax and had gone undiagnosed. So for his next round of treatment, we will focus our efforts on his MCL to finally stabilize the knee. If you’d like more information about how this type of biomechanical approach is changing the way we diagnose and treat patients, see our medical practice’s e-book, Orthopedics 2.0.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.