Physician Based Innovation Scores Again: Gastric Bypass Surgery Beats Meds in Study after Study
There are two pathways for medical innovation, physician based innovation and pharma based innovation. However, based on the news media’s coverage of stem cells, you wouldn’t really know it. Whether it’s stem cells or stomach surgeries, physicians have created many of the best medical care we have today.
In the 1980s, shortly after I graduated from medical school. I would see billboards of doctors advertising for gastric bypass surgery for weight loss. At the time, seeing any advertising by a physician was a new concept. In addition, this all seemed counter to the news on the topic, which was uniformly negative. Reporters often pointed out that the procedures weren’t covered by insurance and could run tens of thousands of dollars. They noted that the risk of the procedures could be high and that no one was sure of the possible long-term effects. Finally, they would also point out that no university scientists had yet blessed these procedures. However, the doctors who were performing gastric bypass saw that it worked to help very obese patients lose weight and live a more normal lifestyle. What began as a few physicians, soon morphed into hundreds and then thousands of physicians performing the procedure. Professional societies were launched to establish guidelines. Small case series were first published. Then came larger case series and complications papers. This was followed by comparison trials and finally randomized controlled trials (RCTs). Where is all of this today? This last 2 years, in RCT after RCT, these surgeries have destroyed medications for treating type 2 diabetes. The studies haven’t even been close. Basically, in the groups treated with gastric bypass, many patients are cured of type 2 diabetes, whereas in the medication groups, none are ever cured. A new study was just published this week.
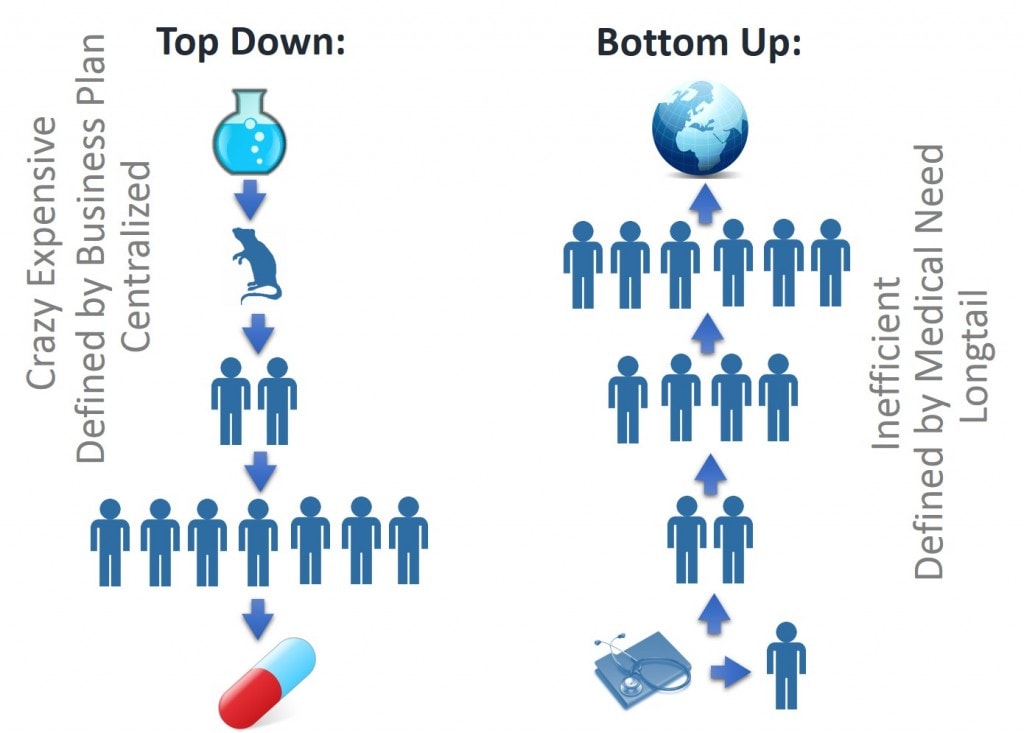
All of this is an apt example of physician based innovation. Physicians innovate very differently than large universities, or what I call the Pharma approach. Physicians see problems on the ground in the patients they treat but can’t help. They then innovate to help those patients (see above). At first, the only evidence of efficacy is that the procedure works in a unique patient, then in more patients. This then leads to small studies which then eventually lead to larger studies. Pharma innovation is different. This process usually begins in the lab. It then moves onto animal studies that show that substance X helps disease Y. The FDA approval process then begins, leading to small studies that lead to larger studies. After a huge expense and about two decades, eventually 1 in 1,000 tested compounds will see the light of day as a prescription drug.
How do the end user costs of the two pathways compare? Because of the massive expense of the Pharma process, the end price of the drug must be very high. For example, the latest diabetes drug can cost thousands of dollars per year to treat diabetes, while curing nobody. The lifetime revenues for pharma companies from a single 45 year old patient can be hundreds of thousands of inflation adjusted dollars. This happens because the drug company has a virtual monopoly granted by the FDA. These days, gastric bypass, developed through the physician innovation process and existing in a free market, can be had for around $7,000. In addition, a large number of patients that undergo this surgery will be cured of their diabetes, never needing to take drugs again.
Gastric bypass surgery is a great example why society needs to protect the physician innovation pathway. Without it, countless therapies that should be developed over the next century won’t ever be developed. For example, the patients who are now being cured of diabetes through gastric bypass surgery, would all still be stuck on expensive and often dangerous meds (many diabetes meds increase heart attack risk). Whether it’s stem cells or stomach stapling surgery, we need physicians innovating in the open market to bring us every possible cure. Without them, we’re stuck with a crazy expensive drug approval process that’s bound to keep stock prices humming, but patients disenfranchised from what works the best.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.