Osteonecrosis Treatment Without Surgery? This Is a Tough One…
Yesterday, I treated a patient at our licensed Grand Cayman advanced practice site who had at least 11 sites of a dreaded disease known as osteonecrosis. Her disease is so severe that she fractured her knee femur bone just by using a kickboard for a single lap in the pool. The orthopedic surgeons back home weren’t quite sure what to do, so we were literally her last hope. In addition, there was no place on earth she could have gotten this many areas treated with this many stem cells.
What Is Osteonecrosis?
Osteonecrosis is where the bone dies and loses its structural support or, put more simply, turns to mush. It’s also known as avascular necrosis, which harkens back to a time when we thought all of this was mostly caused by the lack of blood supply. For the most part, that’s not usually true. Most cases seem to be caused by chemical poisoning of the cells that maintain bone.
The most common causes of osteonecrosis are alcoholism, anti-inflammatory steroid use, osteoporosis drugs, and chemical exposure. Of these, the single most common cause of osteonecrosis that is easily preventable is steroid use. What’s crazy is that if you take a common oral corticosteroid, like Prednisone, for just 10 days, your risk of getting the disease goes up 380%. If you find yourself on this stuff for a year, it goes up more than 21,000%!
The most common place osteonecrosis impacts bone is in the hip. The disease can advance quickly as we’ve seen hips go from a small amount of disease to collapse in a matter of months. Sometimes we’ll see multisite disease where both hips and say a shoulder or a knee are involved. What’s even rarer are cases where there are many, many sites.
My New Multisite Osteonecrosis Patient
The patient is a family doctor who was suspected of having an autoimmune disorder, so she was placed on four months of Prednisone. Ultimately her doctors didn’t think she had the disease and she was taken off the drug, but a few months later, she began to have left knee pain. When an MRI showed osteonecrosis, this began an odyssey of increased pain in other areas and finally osteonecrosis being diagnosed in both knee femoral condyles, both tibias, both ankle talus bones, both wrists, both shoulders, and one distal radius. Her disease is so severe that she fractured her knee femoral condyle by trying a lap in the pool with a kickboard.
So what can be done for this patient? Well, traditional orthopedic surgeries like core decompression and bone grafting are out of the question due to the number of sites and the fact that some can’t be treated this way. We’ve been using bone marrow concentrate (a same-day stem cell procedure) to treat osteonecrosis of the hips, knees, and shoulders for more than a decade. We’ve treated hundreds of patients through intra-osseous injection (into the bone), but there is no way to get enough material to inject all of these sites at once. While you could try other cell types, like fat, stromal vascular fraction is illegal in the U.S., and 99% of the world’s research on stem cells healing osteonecrosis lesions used bone marrow stem cells.
Ex-US Stem Cell Options
What this patient needed was the ability to grow stem cells in culture to bigger numbers. While that’s available at different sites around the world, regrettably, there is a steep drop-off in physician skill once you leave the U.S., and that’s reflected in these clinics. As I’ve blogged before, when you go to a Banana Republic stem cell clinic, you get the local yocal doctor as U.S. physicians aren’t allowed to be licensed in these countries.
The other issue here is that there is no advantage to open orthopedic surgery to place stem cells in these sites as this just adds risk multiplied times 11. All that’s required based on the existing research is getting the stem cells to the spot, which can be done through a precise injection into the bone using fluoroscopy. The problem is that even in Europe, the number of physicians who have experience in this type of bone injection would be few and far between. In fact, there are only a handful of physicians in the U.S. and elsewhere who have performed these procedures and likely none have done this many sites.
In the final analysis, the only place on the face of the earth that could culture expand her bone marrow cells (i.e., grow them to bigger numbers to cover all of the areas) and had US licensed physicians who had done many of these bone-injection procedures was our licensed Grand Cayman Advanced Stem Cell Practice site. Hence, the above images. Let me explain.
The Images
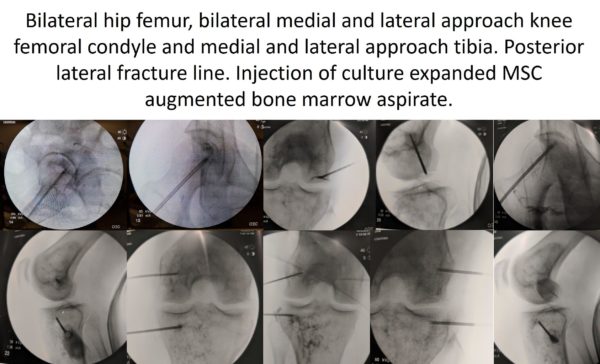
Due to the number of sites that needed to be treated asap (meaning waiting with this disease is almost always a bad thing), we decided to focus on the four knee bones and two hip bones (6/11 sites) this trip. The images above show precisely placed trocars into the hip femur bones with one of those also showing the radiographic contrast in the osteonecrosis lesion (top left). The other images are of microtrocars placed into the knee bone sites. This was two per bone, one on each side. I also injected that fracture line from the kickboarding incident.
The upshot? In the end, I’m proud to say that, hopefully, we will be able to help this poor woman. We are literally her last option. While she has the other sites left to treat, hopefully by early summer we’ll know how all of this is working.
The Regenexx-C procedure is not approved by the USFDA and is only offered in countries via license where culture-expanded autologous cells are permitted via local regulations.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.