Deltoid Ligament Injury and Stem Cells: Understanding Biomechanics of the Ankle
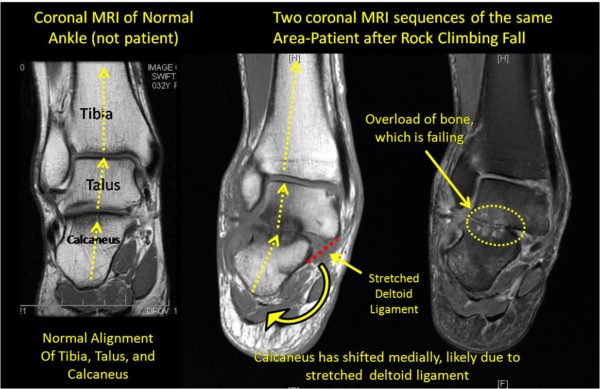
SA is 55 yo WF from Washington state who was seen this morning for an ankle problem that began after a climbing fall last year. She had multiple ankle ligament sprains as well as bone chips floating around. After two surgical debridements (last surgery about 10 months ago), she’s not much better. As I have blogged before, Orthopedics 2.0 is about more than better tools like stem cells or PRP or the next best cartilage replacement or repair technology. It’s also about spending time figuring out how the patient got to the point of having a bad joint and if anything needs to be done to fix those biomechanics before work starts on possible joint repair. JA is a good example. I have included MRI’s above that show (on the far left) a normal ankle alignment between the tibia-talus-calcaneus (normal ankle MRI from someone else-not the patient). Notice that the force lines (dotted yellow lines, pointing up, are relatively straight as the force moves from the calcaneus (heel bone) to the talus (ankle bone) to the tbia (lower leg bone). In this patent’s MRI’s in the middle and on the right (same coronal MRI slice-but different types of MRI sequences), you can see how the force line is skewed to the left. The calcaneus (heel bone) is shifted laterally (in these images-to the left) and as a result there is overload of the bones and talo-calcaneal joint (the yellow dashed line on the far right picture showing light color in the otherwise dark bone). So in summary, because the heel bone is now bent to the lateral side (left in the above pictures), the forces now don’t hit the talus bone evenly. Instead, the lateral talus and heel bone (calcaneus) are overloaded on this MRI and the bone is so beat up, it’s actually starting to die off (the dark color in the bone on the middle picture and the light color in the bone on the right picture). So how did the ankle get this way? Her exam revealed a loose deltoid ligament, which I’ve drawn in above in the middle picture as a red dashed line (“stretched deltoid ligament) above. Think of this as duct tape that normally doesn’t allow the heel bone to move to the left (lateral). When this got stretched in her climbing fall, it all of a sudden allowed her heel bone to move that direction and redistributed the forces to the lateral side of that joint. So in order to fix this (with whatever–we use injected mesenchymal stem cells, others might use different tools), you have to shore up the lateral sub-talar joint (for us injecting her own stem cells into that joint) as well as tighten the deltoid ligament to try and prevent the overload from happening. So orthopedics 2.0 is about more than quick surgical fixes, it’s about figuring out how the joint got to it’s current condition and then designing strategies using advanced tools (such as stem cells) to try and restore normal joint function. What are the surgical alternatives? Perhaps trying to suture the deltoid ligament or a sub-talar ankle fusion, neither is optimal for her desired activity levels.
This patient was treated with the Regenexx-C (cultured stem cell injections).

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.