Does Rotator Cuff Surgery Work?
Does rotator cuff surgery work? You would think that because this has become a standard of care for nonhealing rotator cuff tears that we would have loads of high-level research showing this procedure is effective. However, we really don’t have that research. In fact, we have studies showing that this approach of sewing up a rotator cuff tear may be no better than physical therapy. Now a new meta-analysis shows just how poorly surgery fares.
What Is a Full-Thickness Rotator Cuff Tear?
Chu KyungMin/Shutterstock
Though tears in the rotator cuff are common, finding out that you have one can be concerning—a torn anything just sounds bad—so on the surface it might seem logical that your doctor would recommend surgery to “fix” it. If the word “full-thickness” is used to describe that rotator cuff tear, your first instinct might be to get that surgery scheduled asap. So what exactly is a rotator cuff tear, and what does it mean when your MRI shows a full-thickness rotator cuff tear?
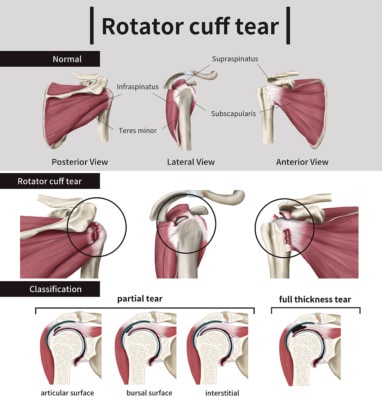
A rotator cuff tear is damage in the rotator cuff (the complex of muscles and tendons that make up the shoulder). These tears are classified based on whether they are partial (not completely through the tendon) or full-thickness (completely through the tendon). Full-thickness tears can also be either retracted (snapped back from the bone) or nonretracted (not snapped back from the bone), which is terminology you might see on the MRI.
While a full-thickness tear is more severe than a partial tear, it doesn’t mean surgery is a given. In fact, whether you have surgical or nonsurgical treatment on those full-thickness tears, there are mounds of research suggesting rotator cuff improvement is the same. Let’s review.
Why Surgery When Rotator Cuff Tears Improve Without It?
A new study of studies (a meta-analysis of 57 randomized controlled trials [RCTs]) found that full-thickness rotator cuff tears improved with or without surgery. Did you catch that? With or without surgery! If patients are experiencing sustained improvement in their full thickness rotator cuff tears whether they receive surgical or nonsurgical treatment, what’s the point of the surgery?
Let’s take a minute and let that sink in. In this meta-analysis of 57 different high-level studies, surgical repair did no better than PT or no treatment! YIKES! Why isn’t this study being talked about in the New York Times or on every major media outlet? Why are insurers still covering these procedures?
No Benefit in That Study, Does Rotator Cuff Surgery Work in Others?
Study after study continues to reflect the same results as the 57 RCTs reviewed in the study above: this recent one also supports that nonsurgical treatment for rotator cuff tears is just as effective long-term as surgery. Despite this, surgeons are still performing these surgeries to the tune of roughly 40,000 per year in the U.S. alone.
More Problems with Rotator Cuff Surgery
Rotator cuff surgeries also come with significant downtime as well as painful rehabilitation intended to help patients regain strength and range of motion, yet one study found that one in three of those who undergo rotator cuff surgery don’t completely heal. Additionally, a disturbing 60% of patients with large rotator cuff tears experience retears after surgery.
Athletes who suffer rotator cuff tears can be particularly vulnerable to the adverse effects of surgery, especially those, such as football or baseball players, who rely on full shoulder function in order to continue to play. Unfortunately, many opt for rotator cuff surgery thinking they’ll enjoy a quick and full return to the game, but the reality is that recovery is lengthy and about half never achieve their preinjury levels of performance.
And what about that shoulder pain? After all, that’s usually what drives a patient with a rotator cuff tear to finally make the decision for surgery. Shoulder pain and that rotator cuff tear actually may not even be related; this is especially true if you are middle-aged or older as tears can occur with normal aging wear and tear.
Is There a Nonsurgical Alternative?
Yes, we treat many rotator cuff tears with precise ultrasound guided stem cells sourced from the patient. For more info on how that’s done, see the video below:
The upshot? This study went unnoticed but was a very big deal. In any other specialty, a large meta-analysis like this would force a reassessment of clinical guidelines. The problem? Removing rotator surgery from orthopedic operating rooms would mean that the hospital couldn’t pay the light bill!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.