Cartilage is “Alive”…
I’ve been spending time catching up on imaging analysis of our >12 month research patient follow-ups (mostly 1-2 years out from their procedure), so expect to see more posted here this next few days-weeks.
The cartilage in the knee is interesting stuff. It’s made of cells that were once thought to be just inert material that could be cut away at will with little implication. Somewhere in the last quarter of the 20th century researchers realized that this stuff was alive. Cartilage is not only living, but also produces GAG’s or glycosaminoglycans. These GAG’s allow for lubrication and help the cartilage to hold onto water. Once the cells in the cartilage begin to die off, they produce less GAG’s and thus the cartilage gets dried out. While a lot is known about catabolic enzymes breaking down cartilage, the real story may be in the balance of break down (catabolic) and repair (anabolic). This is a tale we’ve only just begun to hear, as the explosion of research into progenitor cells helps fill out the chapters of this book. Every time we do something like go for a run, a certain number of cartilage cells perish. Those cells are replaced by mesenchymal stem cells differentiating into new cartilage cells. When the amount of damage exceeds repair, we get cartilage dying off (catabolic>anabolic). When the balance is opposite so that repair ability exceeds damage (anabolic>catabolic), we get a healthy knee.
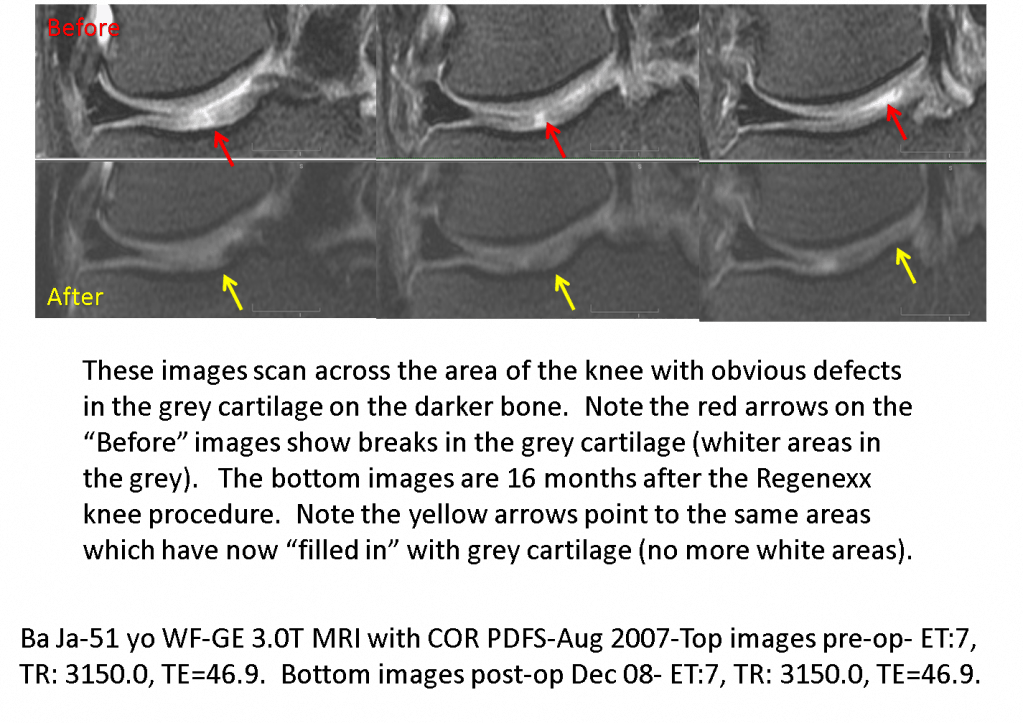
This is the story of a 50 something woman who had a knee MRI showing arthritis. She went in for an arthroscopic clean-up (debridement) about a year and half before seeing us. When she woke up from the procedure the surgeon told her the damage was worse than suspected and that micro fracture had been performed. The patient was placed on crutches for 6-12 weeks and had to cancel a big planned vacation. The knee grew worse over the 18 months between the surgery and our first visit. The biggest issue on her pre-study MRI were the big breaks in the tibial plateau cartilage (the grey stuff below where the red arrows point). The patient had to give up hiking her dog in the hills of Boulder.
The patient underwent the Regenexx-C knee procedure and below are pre-procedure and 16 month post procedure MRI’s. Note the red arrows point to breaks in the cartilage (white breaks in the grey cartilage) in the “Before” image and in the after image, the yellow arrows point to grey cartilage without breaks.
Since cartilage is living tissue, we have to treat it as such. Too often we medical types inject massive doses of corticosteroid (while the body would be used to nanograms, for some unknown reason we inject milligrams-1 million times more). For the living cartilage this is like trying to put in a thumbtack in with a sledgehammer, you can do it, but it “aint” pretty. Hyaluronic acid (SynVisc, Hyalgan, OrthoVisc, Supartz) is a great next step, likely doesn’t heal much but likely helps protect the cartilage (WD-40 for the knee). The next step beyond WD-40? Repair.
This patient was treated with the Regenexx-C (cultured stem cell injections). It should be noted that not every patient with a break in their knee cartilage would be expected to do as well as this patient.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.