A Patient from Our Rotator Cuff Stem Cell Injection RCT
We’ve been slowly recruiting for a randomized controlled trial for the last few years that compares rotator cuff tears treated with a precise injection of high-dose bone marrow concentrate (HD-BMC) with physical therapy. This morning I’d like to update everyone on where the Rotator Cuff Stem Cell Injection RCT study stands and show a before and after MRI image (above). I’d also like to predict the future of traditional surgery by looking back into our past.
Treating Rotator Cuff Tears with Stem Cells
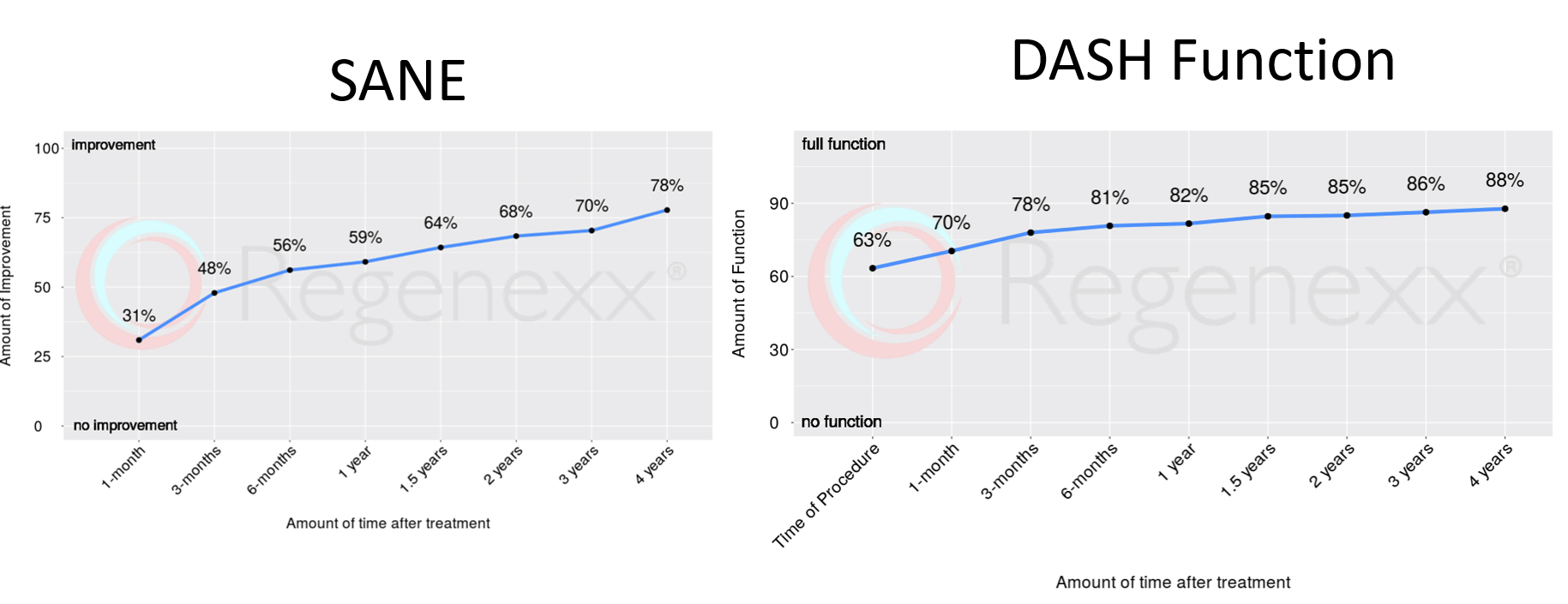
We published on a case series of more than 100 shoulder patients treated with precise high-dose BMC back in 2015. The results were excellent, and as of this morning, looking at our live registry-based outcome data, we’re tracking just under a thousand treated shoulder patients (n=968). In addition, the results are still excellent. Below I’ve shown the SANE scores (percentage reported improvement) and the functional score we use (DASH). In both of these metrics, more is better on the graph.
An Update on our Rotator Cuff Stem Cell Injection RCT
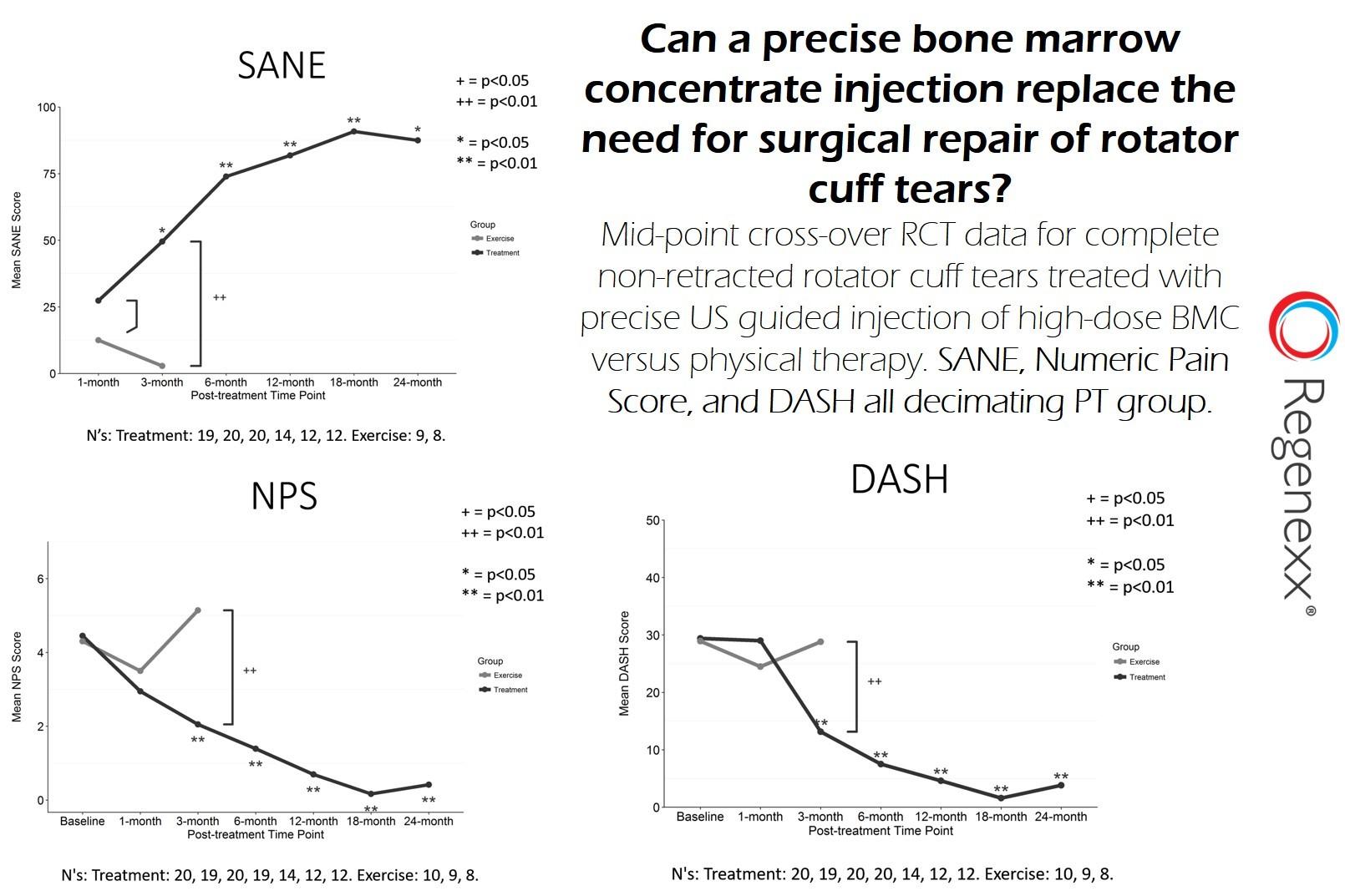
RCT stands for randomized controlled trial. In this case, we randomized rotator cuff tear patients to either get a precise HD-BMC injection or a physical therapy (PT) routine. We have recruited enough patients to satisfy the control group (PT), so every patient now will get the treatment. Below are some of the results to date comparing the two:
The results? They are excellent.
An MRI from That Study
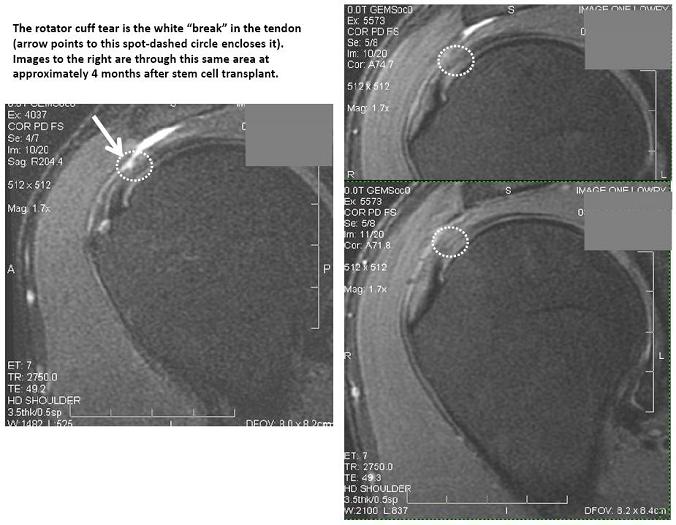
Above is a sample MRI from the RCT, a before and after image that was taken of one of Dr. Markle’s patients. Note the white areas in the white dashed oval. These represent tearing. Also note that in the after image, these have disappeared. They’re now replaced by a dark tendon, which is more consistent with normal tendon. In fact, the reading radiologist read this one out as normal.
An MRI from Ancient History
We pioneered this precise injection-based treatment technique for shoulder rotator cuff tears. Want proof? Below is the first shoulder MRI we reviewed on a patient who we treated with a precise stem cell injection. This was way back in 2007, long before any physicians in the U.S. had even heard of injecting stem cells to treat tendon tears.
The Future?
It’s pretty clear to me based on what I’ve seen over the last 13 years and our published research and Rotator Cuff Stem Cell Injection RCT results that traditional shoulder rotator cuff repair surgery is about to take a serious haircut. That includes a bevy of device manufacturers in this space who make everything from resorbable anchors to arthroscopy equipment. Why? Larger partial-thickness and complete nonretracted tears don’t require surgery. Instead, they can be healed with just a precise high-dose bone marrow concentrate injection. While surgeons dream of getting to perform their surgeries and then throwing magic stem cell pixie dust into the area upon closing, there’s a big problem with that approach. It’s cost plus, meaning the cost of the surgery, plus the cost of anesthesia, plus the cost of a surgery center, plus the cost of equipment and devices, plus the cost of the stem cells. That will never be able to compete financially with an outpatient injection procedure. In addition, the latter has far fewer costs related to complications and side effects.
The upshot? After more than a decade using imaging guidance to precisely inject stem cells into torn rotator cuffs, I’ve learned a thing or two. The biggest lesson this work has taught me is that in the future, rotator cuff surgery rates will fall by at least half. So if you’re a surgeon, begin retraining. The IOF has some great courses in precise ultrasound- and fluoro-guided shoulder injections. Change is good…

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.