What is Platelet Lysate?
You may have heard of platelet rich plasma or PRP, which is concentrating blood platelets and injecting them to prompt healing. Platelet lysate (PL) is it’s more advanced cousin. We first began using PL in orthopedic injuries in 2005. It’s just now starting to catch on via other clinics trying to replicate what we do, so what is platelet lysate and why is it important?
Platelets live in your blood. They are little fragments of cells that are stocked with growth factors and initiate clotting. When you get a cut, it bleeds and the platelets are nanomachines that help to stop the bleeding via a blood clot. The clot is more than just glue to stop the flow of blood out of damaged vessels, it’s also nature’s advanced biologic scaffold to initiate and support healing. Within that healing matrix are billions of platelets that excrete growth factors. These specialized chemicals “speak” to other cells, telling them what to do and energizing the construction effort. I like to tell patients that these growth factors inside platelets act like espresso shots for the cells that are repairing damaged tissue.
PRP is simply concentrating the platelets in the blood. The 1st generation PRPs were messy and bloody affairs that were red and newer PRPs are amber, having eliminated the pro-inflammatory red and white blood cells. Our 2nd generation PRP can be concentrated to ultra-high levels, so we call it SCP (Super Concentrated Platelets). PRP works by concentrated platelets slowly releasing growth factors over approximately a week. Sort of like a timed release version of a pill. What if you want an immediate release version with many more growth factors available all at once? You use a platelet lysate (PL). In our experience while PRP can cause inflammation, PL is very anti-inflammatory and hence can be used more easily around nerves. To get a visual understanding of a platelet lysate, click on the video above.
We began using PL in 2005 as an adjunct to our stem cell treatments. When we began culturing mesenchymal stem cells (MSCs) we didn’t want to use recombinant growth factors or fetal calf blood to get MSCs to grow because of the patient risks, hence we used the growth factors from the patient’s own platelets. Through the years we found some great clinical uses for PL such as to replace toxic, high dose steroids in epidural injections and nerve hydro-dissection. This past 1-2 years, after being the only clinic using PL in the U.S. we’ve begin to see some other clinics begin to use it in patients. We welcome the company, but as usual these clinics are using an outdated method to make PL that’s simple for the clinic, but not the best method for the patient. Let me explain.
The simplest way to make PL is to take red blood cell free PRP (amber PRP) and throw it overnight in the freezer. When you thaw the sample, the ice crystals will have broken up some of the platelets and release the growth factors into the serum. There are some other tricks that most clinics using PL don’t understand, but at least this is a rough and dirty way to get to a PL. Through the years we wondered if this actually broke open all of the platelets, or just some of them? In addition, could we develop a PL that had much higher growth factor content?
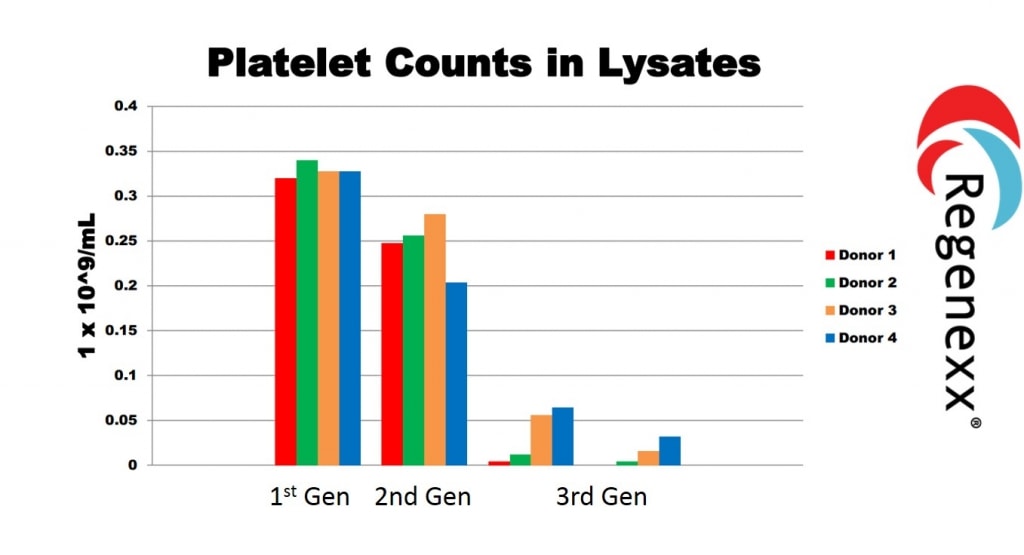
The graph below shows what happens when you put our amber PRP in the freezer to create PL (1st generation). You still have a huge number of platelets that don’t give up their payloads (here noted as 1st Gen). Note that by the time we had created our 3rd generation PL procedure, this issue had been solved (3rd gen). Why? In that procedure, there are few remaining platelets, hence we’ve been able to lyse (break open) almost all the platelets in the sample.
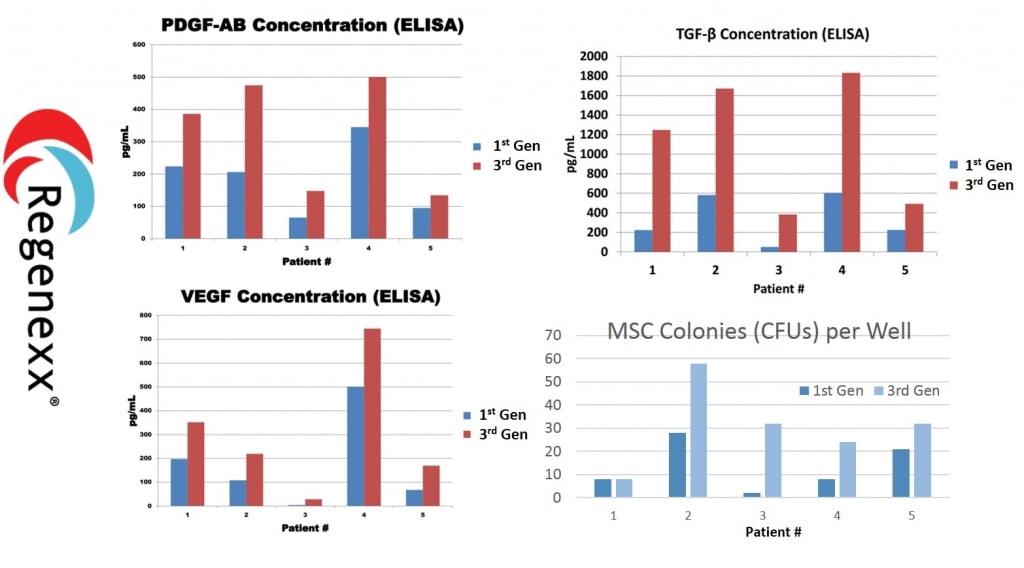
What are you looking at above? The three graphs marked PDGF-AB, VEGF, and TGF-B are all ELISA tests that we ran on our 1st generation versus our third generation platelet lysate. The height of the blue bars equals the growth factor levels in our 1st gen procedure and the height of the red bars are the amounts in our 3rd gen procedure. Across multiple patients we were able to significantly increase the growth factor levels by using a more sophisticated PL procedure (3rd gen). The graph in the lower right corner is what the first gen and third gen procedures do to stem cells. meaning, the higher the bars in this graph, the more stem cell growth we saw in culture. In 4/5 patients tested, there was dramatically better stem cell growth when the 3rd gen procedure is used.
The upshot? As I’ve said before, this is how we roll. While the rest of the world is struggling to figure out how to make a first generation platelet lysate, we’ve been using our third generation procedure for two years and are now working on the fourth generation procedure. Why spend all of this money on continually improving what we do at Regenexx? So that you know that when you get a Regenexx procedure, you’re getting the latest and greatest technology available, not yesterday’s news…

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.