Shoulder Dislocation Surgery Pros and Cons?
What are the shoulder dislocation surgery pros and cons? If you’ve dislocated your shoulder and you see a surgeon, most will argue that you need surgery to fix the bone trauma, labrum, and ligaments. However, do you really need this procedure? Here we’ll explore all of your options as well as newer nonsurgical orthobiologic options.
Shoulder Anatomy
Udaix/Shutterstock
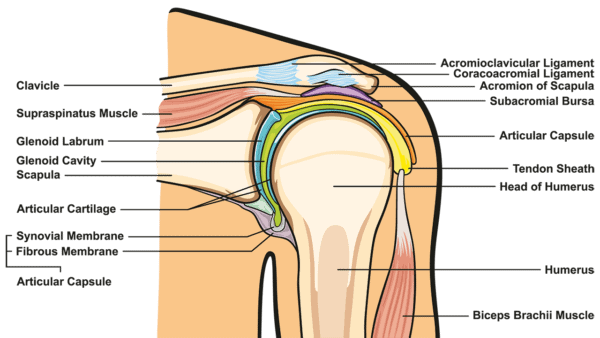
This picture to the left is looking down into the socket of the shoulder joint. I like this image because it shows you how the ball of the main arm bone, called the humerus, (which fits in here) is surrounded by a labrum, the shoulder capsule with its ligaments, and the rotator cuff muscles. All three of these critical structures act in concert to keep the ball in the shallow socket.
Let’s delve into these three structures. The labrum is the lip around the socket and helps to stabilize the ball. Then there’s the shoulder capsule, which surrounds the joint and has several areas of thickening. These all act to both allow movement and prevent the shoulder from dislocating. Finally, the rotator cuff muscles (shown here in red) also surround the shoulder just outside of the capsule and provide both passive stability and actively move your shoulder.
What Is Shoulder Dislocation?
The shoulder joint is a ball with a shallow socket. This allows lots of motion, which is needed so that you can maximally use your arms and hand. However, all of this motion comes at a price. The shoulder is inherently unstable.
Shoulder instability is surprisingly common. In fact, we often see small amounts of shoulder instability that commonly lead to shoulder labral tears, but these often go undetected. How does this happen? Watch my short video below:
What’s less common is when the shoulder joint dislocates. This means that the ball pushes out of the socket because one or more of the stabilizing structures gets damaged. This is the situation where the question of shoulder surgery dislocation pros and cons comes up.
What Is a Bankart Lesion?
When the shoulder dislocates, the labrum or the surrounding bone can be damaged. This tends to happen in a specific portion of the shoulder joint. When this problem is diagnosed, it’s called a Bankart lesion. The surgical knee jerk is that these lesions need to be fixed or the shoulder will have problems down the road. However, let’s explore that a bit more.
Surgery Can Prevent Dislocations
One of the reasons to consider surgical repair of a Bankart or other lesion that allows dislocation is that there’s research to support the idea that surgery can prevent future dislocations. Given that major dislocations can be awful and scary, there’s big pressure to get surgery. However, is there a way to get rid of dislocations without the big surgery?
You Don’t Need Surgery to Prevent Dislocations?
Is there another way? We’ve treated patients for many years through precise injections of platelet-rich plasma or stem cells into the damaged labrum, ligaments, or rotator cuff tendons. We’ve seen patients go from frequent to very rare or no dislocations. How does this work? By tightening down the existing structures that can prevent dislocations. Unlike surgery, there is minimal downtime.
Does Surgery Prevent Arthritis?
One of the reasons often provided to pull the trigger on surgery is that this invasive procedure will reduce the likelihood of osteoarthritis. Shoulder arthritis means that the cartilage wears away and the bone changes shape and develops bone spurs. So does getting surgery really help this problem? Not according to the research.
For example, this study looked at 100 shoulders 13 years after they were treated surgically. The research showed that the operated shoulders had just as much arthritis as that reported by other studies in patients who didn’t get surgery. Hence, the authors concluded that the surgery did little to prevent shoulder arthritis in the long run.
The upshot? As you can see, you may or may not need invasive surgery to help reduce or eliminate shoulder dislocations. Either way, surgery won’t reduce the likelihood of shoulder arthritis, which is often the reason that patients are motivated to get the procedure.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.