What Causes Shoulder Arthritis?
What causes shoulder arthritis? See that shoulder x-ray up there with that big bone spur in the bottom of the joint? That scares me. This past month or two, my shoulders have been aching. As a now 50 year old physician who loves to lift weights, maybe this shouldn’t be too surprising? However, I’ve also been having very distinct shoulder instability episodes in an inferior direction. What does that mean? I can feel my shoulders falling downward all of a sudden and the top parts like the rotator cuff getting yanked. Why? Am I in the early stages of shoulder arthritis? Is there something I can do to combat this arthritis?
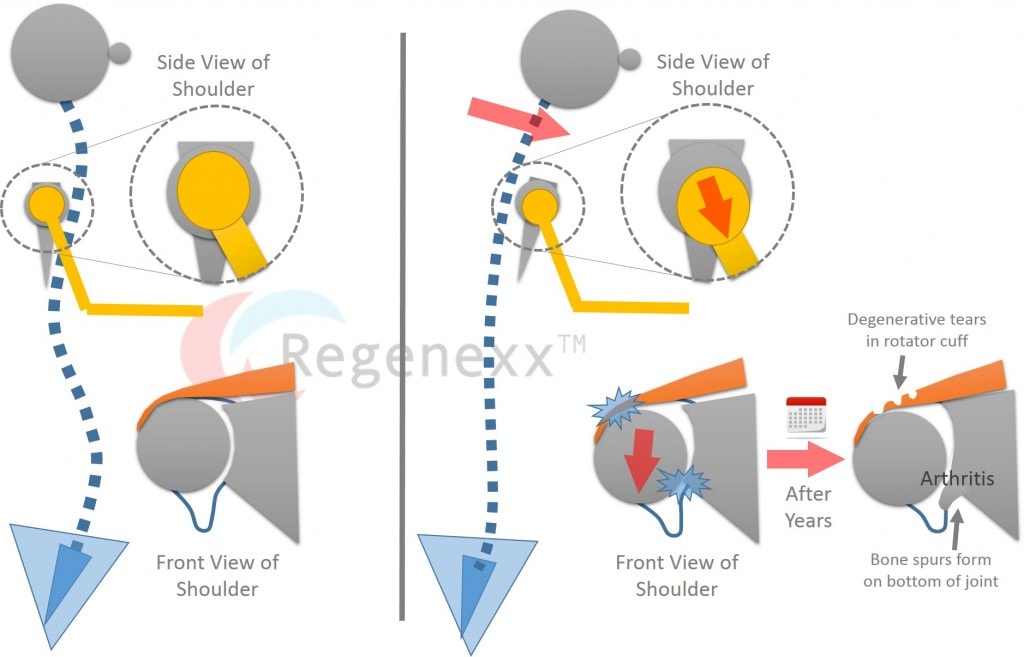
To help you understand what’s happening to my shoulders and what you and I can do to prevent it, I drew some pictures above. When you’re younger, your head and shoulders are straight and aligned with a perfectly balanced spine (neck curve points one way, upper back curve balances it by pointing the other, and your low back goes back the other way)-see left above. Note that the blow up of the side and front views of the normal shoulder on the left has the ball perfectly aligned in the socket. As you get older, your head and shoulders and spine begin to move forward (due to our habit of sitting in chairs). As this progresses, the upper back part of the spine can become kyphotic (hump backed). In fact, this past few months, I’ve been noticing that I now have to catch myself as it’s beginning to feel more natural for me to be in that kyphotic (slouched) position.
What does all of this have to do with my shoulders? As I have become more kyphotic (see right above), my shoulders are beginning to move forward. This has caused the ball of the shoulder joint to fall forward and down, out of the shallow socket. The new position now requires the rotator cuff (red in the front shoulder blow up on the right above) to have to resist that new downward hanging force. In addition, it over stresses the top and bottom of the shoulder capsule ligaments, making me feel a bit like my shoulders are falling off. As this progresses through the years, if I don’t fix the kyphosis, the bottom part of the ball of my shoulder joint will continue to bump into the bottom of the socket. This will cause new bone spurs down there, which will further limit motion. In addition, my rotator cuff muscles will also begin to fail from all of that extra stretching. Finally, this new shoulder position will predispose me to more impingement (where the rotator cuff and biceps tendon get pinched).
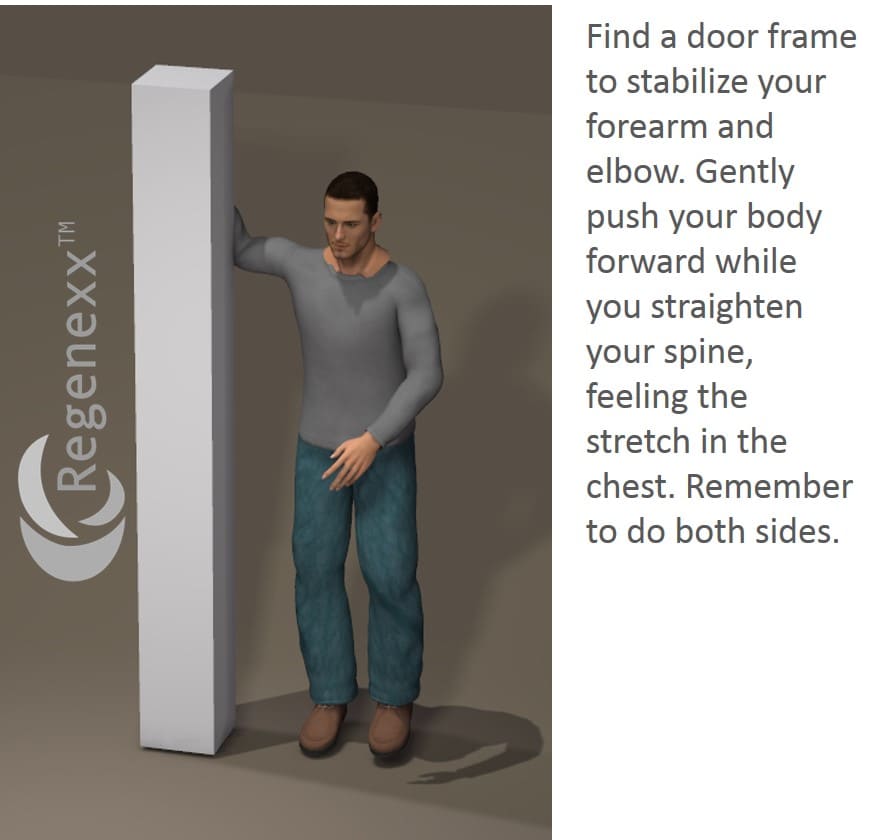
So what can I/you do? First, in the early phases of this kyphosis, you can beat it by using constant stretching against the grain of the forward head and shoulder movement. Here are some of my personal favorites:
In the later phases (once the spine bones have changed shape), you’ll likely need professional help. In any case, if these stretches into extension cause significant neck, upper back, or lower back pain, you may have already had bone changes. Another possibility is that the facet joints in your spine may be arthritic or painful. Either way, you’ll need to see a physician like those in the RegenexxNetwork if this is happening.
Are there regenerative injection treatments? If the shoulder ligaments on the bottom of the joint are lax, injections to tighten these ligaments (like the IGHL) can be very helpful. In addition, if the main shoulder joint has arthritis, stem cell injections into the joint may help. The same holds true for degenerative tears in the rotator cuff, which based on our treatment registry data, respond very well to precise stem cell injections.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.