What Is Foraminal Stenosis?
What is foraminal stenosis? Is it necessarily the cause of your back or neck pain, and does foraminal stenosis require surgery? Let’s start from the beginning…
Your spinal column, or backbone, is made up of vertebrae, stacked one on top of the other, with a disc between each level to provide cushion and absorb shock. The spinal canal is a tunnel that runs down the column and houses the spinal cord, which has many nerves that transmit muscle commands and take sensory information to the brain. The spinal column also has small holes where the nerves exit, and branch off to other parts of the body. There is one at each level. One hole is called a foramen. The plural is called foramina. Watch the short video above for clear images of what these structures look like.
The foramen is shaped like a tunnel that exits off of the spinal canal, and the spinal nerves for each specific level traverse, or go through, them. When the spine is healthy, these nerves easily traverse the tunnel, properly transmitting sensory information from each part of the body to the brain. When the spine is not healthy, however, this flow of information can be disrupted. This can happen when there is foraminal stenosis.
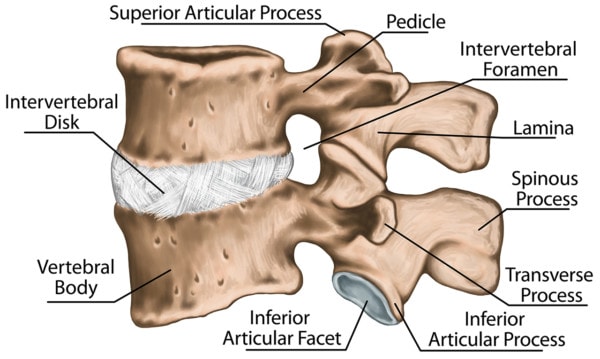
Stihii/Shutterstock
What Is Foraminal Stenosis?
The disc, that cushion between the spine bones, can bulge, or the spine joints can get arthritis, causing the foramen to narrow. This neural foraminal narrowing is called foraminal stenosis, and this can cause the nerves to get pinched. The pressure from a pinched nerve can cause muscle tightness, weakness, numbness, tingling, or pain in the specific distribution of that nerve. So, for instance, if there is foraminal stenosis in the level of the lumbar spine where the nerves branch into your leg and down to your toes, you could experience numbness (or one of the other sensations mentioned) all the way down in your big toe. Tingling in your fingers or tightness in the biceps muscle, for example, could be from foraminal stenosis in the level of the cervical spine where the nerves branch into your arm muscles and fingers.
What Are The Symptoms of Foraminal Stenosis?
- Lumbar Stenosis: Muscle tightness, weakness, numbness, tingling, or pain in the leg, buttocks, or feet.
- Cervical Stenosis: Muscle tightness, weakness, numbness, tingling, or pain in the neck, shoulders, arms, or hands.
- Thoracic Stenosis: Muscle tightness, weakness, numbness, tingling, or pain in the upper back or front of your body.
The pain and discomfort can worsen if you sneeze or cough, which can be an indicator that you have this condition.
Foraminal Stenosis, or neural foraminal narrowing, can be diagnosed through:
- a physical examination of your level of pain, reflexes, movement, and muscle strength
- a symptom assessment of whether your symptom matches the symptoms associated with foraminal stenosis
- diagnostic imaging X-rays, MRI scans, CT scans, and tests of nerve conduction to see if the space between your bones has narrowed
What Is The Treatment for Foraminal Stenosis
Additionally, surgery is often performed after diagnosing the problem solely based on findings on an MRI. I’ve shared research before showing that an MRI indicating stenosis isn’t enough to appropriately diagnose that stenosis as the cause of back pain, and because of this, if you have a foraminal stenosis, you really shouldn’t put all your trust in an MRI. Patients may or may not have back pain with a foraminal stenosis, though they may have pain in another location, such as the knee or shoulder. Research also shows that physical therapy is as effective as surgery in relieving stenosis, so why take the risk with surgery? You would not want to undergo something as invasive as surgery if there are less invasive alternatives. Regenexx’s platelet treatments are a less invasive alternative to consider for treating foraminal stenosis that use your own body’s natural healing agents.
I Have Foraminal Stenosis
About two years ago, I began to notice a little numbness in my right thumb. I then woke up one morning and felt a knifelike pain in my left shoulder blade. I was convinced that I had a shoulder problem and had one of my partners inject PRP into that area, which did no good. Also, my left biceps and forearm would cramp and hurt, and when I traveled on planes, my left shoulder would get weak and then recover. I finally got a neck MRI because my neck was stiff. Sure enough, I had foraminal stenosis. What I didn’t do next is important. I didn’t see a spine surgeon. Instead, I had Dr. Schultz at our Colorado office inject our high-dose platelet lysate into the foramen and around the nerve. It took a few injections, but within a week or two, we had the problem managed. I now get periodic injections a few times a year to keep this under control. I can work out at a high level, so I’m fully functional.
To learn more about nonsurgical foraminal stenosis treatment options, see below:
- Kathie’s story: Spinal stenosis treatment alternative helps scuba diver get back in the water
- Treatment success in a patient with foraminal stenosis
- Nonsurgical spinal stenosis alternatives
The upshot? What is foraminal stenosis? It’s a narrowing of the tunnel where the spinal nerve exits, and it causes symptoms in areas of the body controlled by those spinal nerves. However, foraminal stenosis seen on MRI doesn’t automatically mean the stenosis is the cause of your back or neck pain. However, whether it is causing back pain or referring pain, tingling, or weakness somewhere else, it’s a good idea to explore nonsurgical regenerative medicine solutions to treat it before it progresses.
Is Foraminal Stenosis the Same as Spinal Stenosis?
Foraminal stenosis is the narrowing of the opening at the sides of the vertebrae where each spinal nerve exits the spinal canal and goes out into an area of the body. Spinal stenosis is the narrowing of the central spinal canal itself where all the spinal nerves run through. Both foraminal stenosis and spinal stenosis can occur due to herniated discs, degenerative discs, or facet arthritis.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.