Can Stem Cells Help Knee Arthritis?
Can a same day treatment with stem cells help knee arthritis if all of the conditions are right? RM was 56 when we saw him in 2011 and now 3 years later, a new MRI shows some interesting changes. So I thought I’d use his image as a thought experiment this morning to discuss why RM is likely a good stem cell candidate.
We’ve been collecting registry data for many years that fits with our clinical experience that our stem cell protocol helps most patients with knee arthritis. RM is a good example of what we see clinically. He was treated with a same day stem cell procedure for his knee, ankle and hip in 2011. His ankle is still fine, despite a 30 year history of issues. His hip and knee have some pain starting to return after a long hiatus, so he called about a “touch up” treatment. So far, RM seems like the typical Regenexx patient that gets long-term responses to the treatment. However, his knee MRI changes between 2011 and 2014 are what caught my eye.
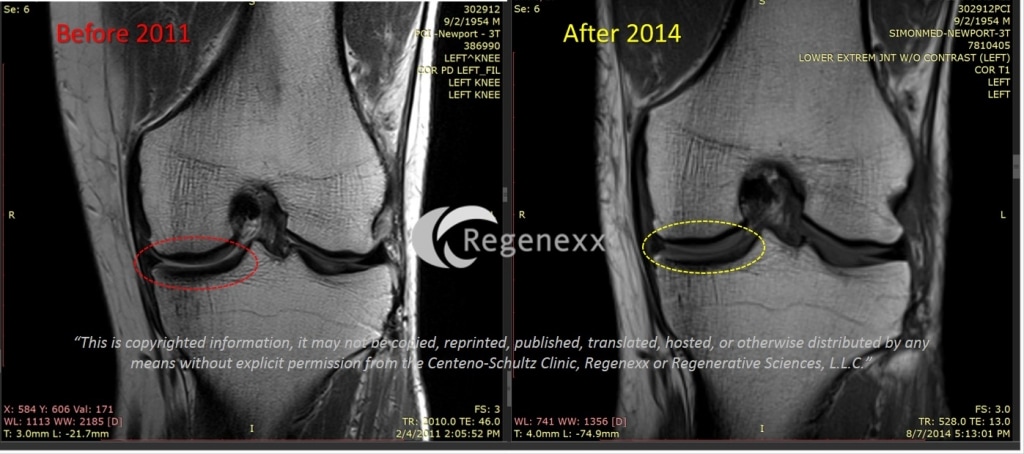
First, while we’ve seen good evidence of MRI changes in conditions such as ACL tears, mild arthritis, meniscus tears, and rotator cuff tears-in moderate to severe arthritis MRI changes with stem cell treatment are less reliable, despite reports of significant improvement in pain and function by the patient. I have blogged a few times on why this may be the case. RM’s pre-procedure film in 2011 on the left above shows mild to moderate arthritis in that the cartilage inside the red dashed circle above is worn down about 50%. However, on the after image on the right, in the same area (yellow dashed circle) the patient now appears to have thicker cartilage (the grey parts). The rest of the MRI is consistent with this positive change. Why?
I’ve extensively looked through data from more than a thousand stem cell patients who have had their knees treated with the Regenexx-SD procedure. While there are some interesting things that predict a worse outcome, I can only rely on a decade’s worth of experience to render an educated guess as to why RM did so well with MRI cartilage changes. One of those is that we started far earlier in this patient than most patients who seek our services. Most patients who come to see us only begin looking for knee replacement alternatives after they’re told they need a knee replacement. By that point their knee is trashed with moderate to severe arthritis. The second reason I think this patient likely did well is blood sugar control. His HBA1C is an enviable 4.9. This metric of insulin control is as good as it gets. We know now through multiple studies that poor blood sugar control, which is an epidemic in our carbohydrate and sugar fueled culture, causes the chemical attack and breakdown of cartilage. Finally, RM may also have been dealt a better genetic hand than most patients. While he did have three joints with arthritis, his knee and ankle were traumatic injuries. Where many patients who have had most of their knee meniscus removed surgically for a tear would have had rapid onset of arthritis in a few years, even before we first evaluated him, RM’s knee cartilage held together much better than most.
The upshot? RM is an interesting example of perhaps how you can optimize your chances of similar results if you are thinking of getting a stem cell treatment for knee arthritis. I believe that the single two biggest things you can do to maximize your outcome are to intervene early and to get your sugar act together. The last part may require working with a physician to cut out the carbs!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.