A Maximally Damaged Ankle and Surprising Results
When I first met Don and he showed me his ankle, I think I said or thought, “Wow!” It was twice as big as his other ankle due to the surgical free flaps, and his MRI looked like a bomb had gone off in his talus bone. When we discussed whether stem cells could help, I think he could read my body language, which loudly said, “Uhhhh, maybe?” That’s why this is a fun blog post to write, as Don ultimately surprised me and then some.
Don’s Ankle
Don fractured his ankle back in the ’80s and had hardware surgically placed to help his damaged bones mend. The ankle then got infected and the hardware was removed, and many surgeries followed, including a free-flap surgery. In this case, that meant taking a muscle from his calf and sewing it over the nonhealing and infected bone to bring more blood supply and healing potential to the area. What he ended up with was an ankle that looked like a tumor had grown around it. That worked reasonably well, until about 3–4 years ago when he began to get arthritis in the main ankle joint. By the time he walked into the clinic for me to check this and other problems, his pain was an 8 out of 10 on medications.
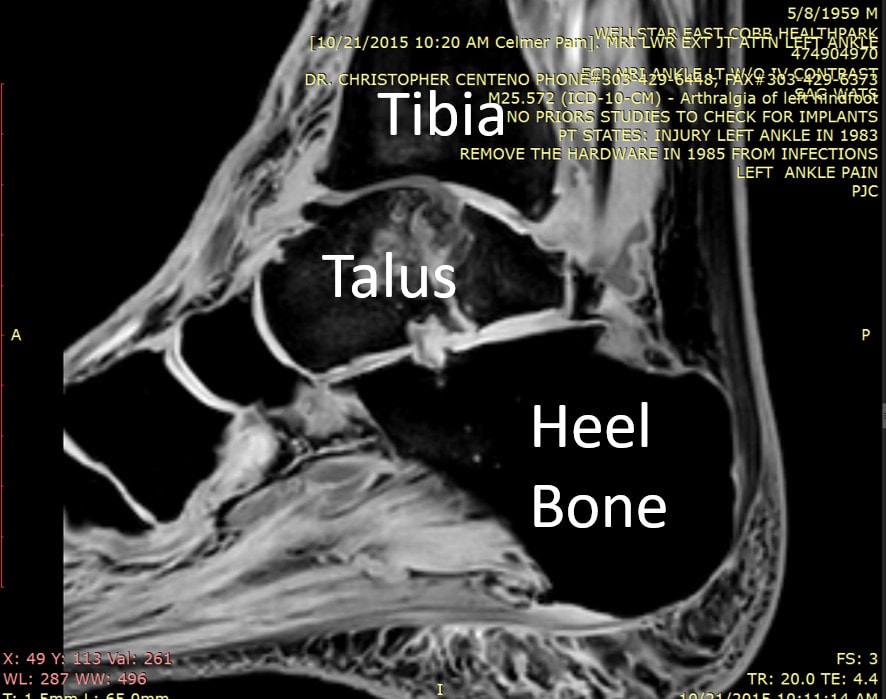
The MRI animated GIF above slices through his ankle sideways. I’ve included one of the slices to the left so you can get oriented. His talus is the oddly shaped bone in the middle, which is where I want you to focus your attention on the image. This bone is one of two (the other being the tibia) that make up the largest ankle joint.
On this type of MRI sequence, the normal bones are black. The bright areas you see in the talus bone above as the slices fly by are areas where the bone is fractured and never fully healed. Any white in this bone is abnormal, but the MRI shows that some of these fractures communicate with the tibiotalar joint, which is not good. In summary, his talus bone is a fragmented mess that never fully healed.
Could we help this ankle?
Don’s Stem Cell Plan
Looking at the severity of what we were dealing with, I steered Don in the direction of cultured stem cells. This means that at our licensed advanced-stem-cell-treatment site in Grand Cayman, we would grow the cells to bigger numbers. This not only made sense for this area, but we had his back and shoulder to treat as well. Using culture expanded cells would make it much more likely that we would have enough cells to treat everything.
I was very concerned that we might have to inject not only into the tibiotalar joint but also into the talus bone. However, that would risk the bone further fragmenting and falling apart; hence, we decided to only treat the joint and hope the cells would make it into the damaged and fragmented bone. This made sense, as there seemed to be actual physical communications between the joint and the pieces of the talus bone.
So how did Don do? He reported to me today that after his treatment in May, some seven months ago, his ankle pain is now down to a 2 out of 10, and he’s off medications. He went skiing this past weekend, and he’s back to activities he couldn’t dream of before. In summary, he did very well.
The upshot? Don’s recovery surprised the heck out of me. However, it goes to show you that even when we place patients in the poor category for a stem cell procedure, sometimes they surprise us. In Don’s case, I’m eager to see a recent MRI and have ordered one. In the meantime, I’m glad that he’s pleasantly surprised and has become our newest Regenexx evangelist!
The Regenexx-C procedure is not approved by the US FDA and is only offered in countries via license where culture-expanded autologous cells are permitted via local regulations.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.