New England Journal of Medicine: R.I.P. Back and Neck Fusion Surgery
There has been an explosion in low back and neck fusion surgeries in the past two decades. However, I often tell my patients that “fusion is a dog with big fleas.” After they have a spinal fusion and are seen in the office and have more pain somewhere else, I tell them that they’re now getting bit by those fleas. Now a new high-level study published in the prestigious New England Journal of Medicine (NEJM) shows that fusions may be on the way out, as they failed to show any clinical value.
What Is a Spinal Fusion?
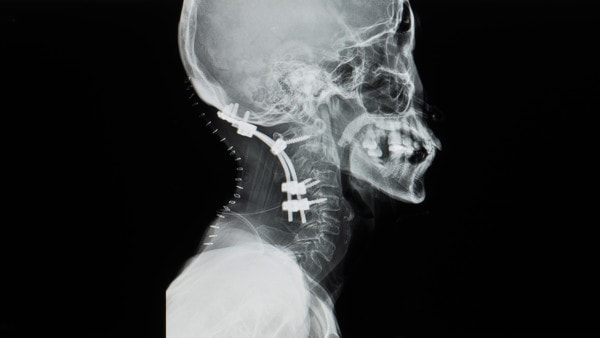
Yok_onepiece/Shutterstock
The spine was built to bend, and as such it has 24 segments or levels that each moves a little bit. A spinal fusion surgery means that one or more levels of the spine are bolted together, usually with screws, plates, or spacers in the disc. Bone is often used to literally grow the discs together.
Why Is a Spinal Fusion Performed?
As the spine degenerates, it gets sloppy and the segments move too much. The idea behind a spinal fusion is that by bolting the spine levels solid, they won’t be able to move. However, does this really solve the problem? Let’s explore that further.
Why Has the Frequency of the Surgery Exploded?
Twenty years ago, spinal fusion surgery was rare. Most patients who had a spinal problem, like a pinched nerve due to arthritis or a disc bulge, only had the bony area pinching nerves opened up surgically (a laminectomy) without a fusion of the operated levels. However, about 15 years ago, fusions became more and more common, and fast-forward to the past few years and most patients who get spinal surgery get offered a fusion. Why?
It’s certainly not because we have high-level research showing that a fusion adds a lot of improvement over the standard surgeries, like laminectomy. In fact, one of the drivers for this explosion has been that adding a fusion reimburses dramatically more from an insurance company than without. Add to that a huge industry that can sell a $5 screw made in China for several thousand dollars and it’s not hard to see why the practice has exploded.
What Are the Downsides?
Given that the spine was designed to be in motion and still needs to move no matter what we do to parts of it, it’s easy to see that locking down any one or more levels just overloads the adjacent levels. In fact, the breakdown of these adjacent segments is so common after spinal fusion that there’s actually now something called “adjacent segment disease” (ASD). This means that because of the fusion, the next level or two up or down degenerates more rapidly due to the lack of motion in the fused area.
Is There Any Evidence That Spinal Fusion Works?
Given the incredible invasiveness of bolting the spine together and the huge cost of these surgeries and the fact that we know that ASD is real, you would think there was incredible evidence that the surgery works. Nope. This week marked the publication of the world’s first randomized controlled trial of lumbar fusion.
In this new study, almost 300 patients with low back spinal stenosis (arthritis that’s putting pressure on nerves) were randomly assigned to undergo either a traditional laminectomy or that surgery plus a lumbar fusion. The result was not surprising—adding a fusion surgery didn’t improve outcomes at two or five years after surgery!
Let’s think about that for a moment. We’re exposing patients to much higher surgical risk by adding a fusion and also placing them at risk for breaking down the adjacent sites of the spine. Without any positive effect of adding the fusion, why are we doing this surgery?
The upshot? Spinal fusion surgery doesn’t help patients; in fact I’ve seen more patients harmed than helped over the last two decades. Now it’s also official: the world’s most prestigious medical journal has now published a high-level study that shows that spinal fusion adds nothing to the average laminectomy surgery. RIP, spinal fusion!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.