The Evidence behind Knee Meniscus Surgery
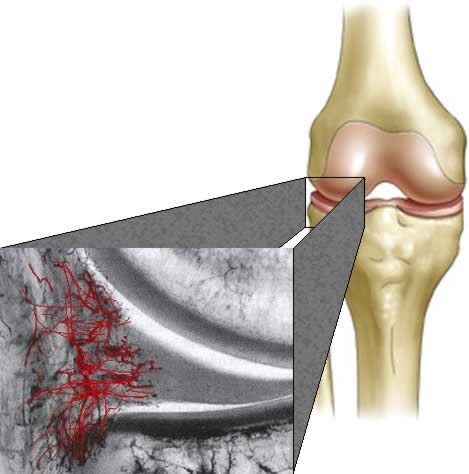
For the past several years and moving forward into the future, we will see many new research studies trying to ascertain if a medical procedure has solid evidence for efficacy. This is often done through a meta-analysis where researchers look at many different published studies. The findings of these studies are often that what is being performed commonly by physicians and surgeons doesn’t have the highest level of evidence (level I). A recent study came to that conclusion regarding arthroscopic surgery of the knee to repair or trim a meniscus tear, concluding that there was no high level evidence showing that it helped patients. The fact that knee surgery didn’t meet this research based criteria for efficacy is not surprising, in that many things physicians do don’t have that level of support. In fact the only surprising thing is that the vast majority of the patients we talk to everyday don’t know that there’s no high level evidence showing that knee surgery to fix a torn meniscus works. While my posts have discussed many reasons why menisectomy likely doesn’t help, including the fact that less knee meniscus tissue (after some has been trimmed out during arthroscopic knee surgery) likely means that arthritis will follow, there are other concerns. One of these is that the meniscus is mostly without blood vessels (avascular) and as a result, won’t heal when sutured. Even when areas of the meniscus with blood vessels are found to be torn and sutured, these areas of the torn knee meniscus that are surgically repaired often fail to heal as well. The diagram above shows the blood vessels in the outer meniscus and the fact that the majority of the meniscus has no blood supply. In experiemental studies, CD34+ stem cells have been able to establish new blood supply in areas without good supply and this may be why we often see good success with many of our patients who recieve injections of their own stem cells into a torn knee meniscus.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.