Transparency in Regenerative Medicine: Is Severe Degenerative Disc Disease a Rare Side Effect of BMC Injection?
Way back when, in 2005, I was the first physician on earth to inject bone marrow concentrate into a degenerated disc. Thirteen years later, there are at least a hundred clinics around the country who use this technique, and many report good results in the right type of patients. However, at Regenexx, we have always been transparent with our results, both good and bad, so this morning I’d like to share one procedure that didn’t end well. Why? Because that’s the right way to practice real medicine.
A History of Showing ALL Results
Through the years, we have always periodically published our results either online or in the peer-reviewed literature. In fact, in 2015, we published the world’s largest safety and complications paper in orthopedic stem cell therapy. That paper had an independent adjudication of all serious adverse events by a star-studded team of physicians who weren’t associated with our company. In the end, it showed that the same-day stem cell procedure (bone marrow concentrate) was very safe relative to the surgical procedures it helped patients avoid. In addition, before that paper, we also published two more on the use of culture-expanded cells in orthopedics, and a third party also published a review of our raw data (see here, here, and here).
At the same time, we have always published some of our patients’ stories who didn’t get the result they desired. Here are only a few of the links that point to these posts:
- A treatment failure in severe hip arthritis
- A failure to heal a knee meniscus injury with the same-day procedure, and a failure of the cultured procedure to improve knee pain in severe knee arthritis in a patient with metabolic syndrome
- A patient with metabolic syndrome and four prior knee surgeries who didn’t get a good result with the cultured procedure
- A treatment failure involving the same-day procedure and severe ankle arthritis
- A patient with a large rotator cuff tear that didn’t heal with the same-day procedure
- A failure of eight weeks to experience any improvement from a knee injection and a mild flare-up
Why post these sprinkled amidst the stories where patients had good results? Because that’s real medicine. Some patients don’t respond, and a few get worse with any treatment.
We’ve also published real-time outcomes for several years now. By clicking on this link, you will see up-to-date outcome data on patients being tracked in our registry. This averages the patients that did well and those who had no response. The good news is that there’s generally more of the former, but if the mean SANE score (Single Assessment Numeric Outcome or percentage improvement) is 70%, you can bet that some patients got great results at 70% and some got lesser results at 50% or less.
Our History of Treating DDD
As discussed above, in 2005 I was the first physician on earth to try to treat degenerative disc disease (DDD) with bone marrow concentrate (a same-day stem cell procedure, or BMC) and then eventually cultured-expanded stem cells. In that time, we’ve treated several hundred patients who have had DDD with orthobiologics including BMC, specially culture-expanded mesenchymal stem cells (MSCs), and high-dose platelet-rich plasma (PRP). During that same time period, we have also treated several thousand low-back-pain patients by staying out of the disc and using platelet lysate or PRP to treat the facets, ligaments, irritated nerves, muscles, and so on. Why so much more of one than the other? Because injecting the disc is always more invasive, and we try to keep patients safe by offering the least invasive therapy that may help their condition. Hence, it’s a testament to how well extra-discal platelet therapy works that we have had so few patients progress to disc injection therapy.
What Are the Routine Side Effects of Disc Injection?
Anytime you inject a patient’s disc, there are two very real and well-known side effects. These are disc degeneration and discitis. The former has been studied through the years with some controversy. The original study showing that poking a hole in the disc to inject something may cause the disc to degenerate in some patients was hotly contested back and forth. For example, at least one study followed young patients who had their disc injected and found no changes at five years.
If just poking a hole and injecting something into the disc causes some discs to degenerate, why would this happen? A few lab-based studies have shown that the radiographic contrast agents that physicians use to ensure that we’re inside the disc on fluoroscopy may have a negative impact on disc cells (also this lab-based study). Also, just the act of poking a hole in a disc to inject anything may also be the culprit in causing some disc degeneration.
Finally, discitis, which is a disc infection, is a rare side effect for every disc injection. This happens in somewhere between 1 in 500 to 1,000 injected discs. If this happens, it’s a big deal, requiring at least IV antibiotics and often surgery.
What Side Effects Have We Seen with Injecting the Disc?
In our 13-year orthobiologic disc injection experience, we haven’t seen many side effects. Generally, the biggest adverse event is that the procedure may not work. I have seen one case of discitis after a PRP injection in one of my patients. I know of at least one other physician, not on our network, who has also reported a single case of discitis with a PRP injection. We also have observed one disc herniation with the culture-expanded procedure that may or may not have been related. Outside of that, not many adverse events have occurred.
What Happened in This Case?
The patient was in a car crash that injured his low back in 2015. He had tried different types of low-back injection procedures prior to his BMC injection. In Feb of 2017, one of our network physicians agreed to inject his L2–L3 and L4–L5 discs. This resulted in a severe flare-up of 10–12 weeks, which is not outside of possible in some patients, but certainly on the high end for the duration of a flare-up. For example, the worst flare I had seen with this injection was a patient who told me that for two months he could barely get out of bed, but then turned the corner and did well. I have one patient who has had severe one- to two-month flare-ups after two back-to-back injections in as many years but eventually reports less pain than before the procedure. However, 90% of patients would have three days to three weeks of increased pain.
After the procedure, he needed to visit urgent care, and they gave him a course of high-dose oral steroids (not advised as this will hurt the injected stem cell population). He also continued to seek traditional interventional spine care for his low back, eventually getting radiofrequency ablation of the facet joints as diagnostic blocks showed that these joints may be causing pain. The network doctor also ordered a one-month MRI to see what was going on. When compared to a 2006 image, there were no changes.
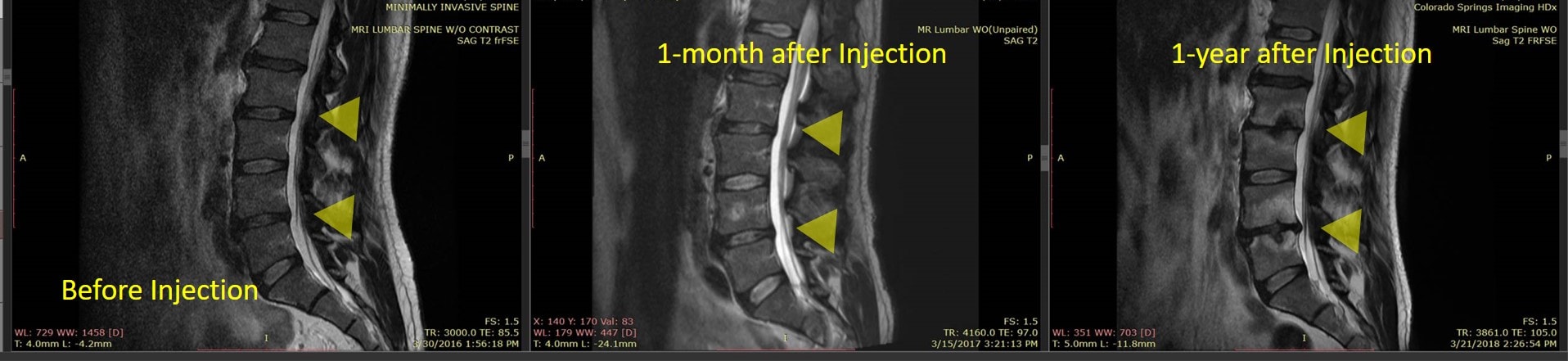
The patient recently sent this one-year MRI. The yellow triangles denote the discs that were injected before, one month after, and one year later. The one-month MRI after the disc injection shows absolutely no changes in the injected discs. However, the one-year MRI after injection shows that now the discs have severely degenerated. So what caused this?
The fact that the one-month MRI shows no disc damage from the injection would argue that it wasn’t the BMC injection. However, at the same time, his increased pain began after that procedure and lasted for a long time for a post-injection flare. While this could have been a sign of discitis, that’s apparently been ruled out. The next part of the analysis needs to take into consideration that we’ve injected hundreds of discs with various orthbiologics and have not yet seen a result like this happen. Hence, on balance, I would say that it’s unlikely that the BMC injection caused this disc degeneration, but that it can’t be ruled out completely. Meaning it’s more likely than not that the damage was done to these discs by the car crash and they just finally gave out. In addition, he also had oral steroids, steroid low-back injections, and RFA, any one of which could have also hastened the demise of these discs.
The upshot? We are transparent. We don’t hide our results; in fact, we publish them every month online and several times a year in the peer-reviewed research. Hence, my goal today was to make sure that if disc degeneration is a rare side effect of orthobiologic disc injection (which is less likely given the fact pattern of this injection), that I cover that topic on the blog.

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.