Rethinking A2M: Hype or Arthritis Miracle Cure or Something Else?
Back in 2015 I posted on A2M, which was peaking in popularity. This is a cytokine that can quench some of the breakdown molecules in degenerating joints. There is a bedside machine on the market that can concentrate this from blood, and many doctors who use it like it. As a result, we developed our own lab-based protocol to try it out. The good news is that we were impressed, but like everything, it seems to work best in specific patient populations and in others not as much. Let me explain.
What Is A2M?
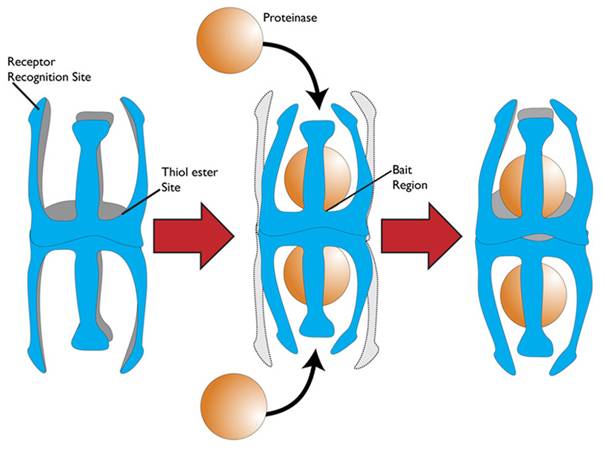
A2M stands for alpha-2-macroglobulin. It’s a very large serum protein that has the unusual function of quenching certain tissue breakdown chemicals. While A2M has been known about for a while, physicians over the last few years have begun to use it in arthritic joints after an animal study was published showing that it can help reduce cartilage breakdown. Specifically, it can inhibit MMP-13, which is a collagen breakdown protein involved in the progression of arthritis.
If you look at the diagram above, the ball represents the MMP-13 molecule, which is trapped on either end of the A2M structure. So one molecule of A2M can get rid of two molecules of the MMP-13 bad guys.
Do We Need to Concentrate A2M?
When I first read the above linked Wang paper that found that A2M can help reduce the levels of a cartilage breakdown chemical and slow arthritis progression, I was intrigued. While the paper gives the amount of A2M needed in chemistry molar format, our lab team converted that to 40 mcg. When we looked at the A2M levels in all of our treatments, like high-dose PRP and our unique same-day stem cell treatment, they all had more A2M than that number from the study. What I didn’t know back then was whether producing a serum with higher A2M levels could be an effective treatment in and of itself.
Creating an A2M Concentration Protocol and Using A2M in Arthritis Patients
Given that we’re Regenexx and we don’t rely on purpose built machines that only do one thing and use instead a flexible lab platform capable of many things, we can create new protocols to isolate new things. To create and validate an A2M protocol, we tried a number of different methods. We tested the pros and cons of each and finally settled on a way to concentrate the protein to 6 times over baseline.
Once we knew how to create an A2M-rich serum, the question became, who will this help? After using it for a year-plus at our Colorado clinic, it seems to work well in two patient types:
- Patients with metabolic syndrome who have severe swelling in joints. These patients tend to be heavier and have big joint effusions. Why? These patients tend to have a high inflammatory environment, one where A2M performs well.
- Patients whose arthritis doesn’t respond well to high-dose PRP. While these patients are fewer and farther between, A2M seems to help these joints.
Outside of that, A2M seemed to underperform in other areas where high-dose PRP or a same-day stem cell procedure worked well.
How About Chondroprotection?
Theoretically, based on the animal studies, A2M should be able to protect cartilage from breakdown after the joint has begun to deteriorate. There really is no easy way to tell if this will work in human patients, but we have begun to try this in select active patients who want to keep their joints healthy. Only time will tell if this strategy works.
A Super A2M Mix?
It should also be noted that other studies have shown that PRP can help reduce cartilage breakdown. In this case, this likely works through stimulating cartilage growth. Hence, for patients in whom we are trying to protect cartilage, we may combine A2M with a high-dose PRP.
The upshot? We’ve begun rethinking A2M. We’ve now seen it work in a select group of patients, and as a result, we’ve begun to use more of it. In the meantime, we’re also now using it combined with high-dose PRP to help active patients stay active. While that last use is harder to quantify as these patients don’t generally have a lot of pain, we hope that their results look more like the animal studies in that their joints get some protection from cartilage breakdown!

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.