Can a Precise Stem Cell Injection Work Where Surgery Fears to Tread?
A patient recently came to us with a very serious problem. She had not only a shoulder bone (humerus) fracture, but also osteonecrosis. Her orthopedic surgeons had told her that trying to get this to heal would be like trying to bolt tissue paper to tissue paper and consequently there was no surgical solution. As a result, she traveled to see us in Colorado to see if new up and coming interventional orthopedics techniques using stem cells could help save her shoulder.
To understand how bad this shoulder was you have to understand a few things about bone. We’ve all had a fracture or know someone who has had one, so we know that bone generally heals in about 6-12 weeks. However, in certain rare circumstances, bone can’t heal. This is called a non-union fracture. In addition, another horrible disease is called osteonecrosis (a.k.a. avascular necrosis or AVN). This is where the bone itself begins to turn to mush, usually due to a lack of viable local stem cells to maintain that bone. What happens if you have both at the same time? Trying to bolt the fracture together after placing some new bone in the area (a bone graft with internal fixation) won’t work, as there isn’t much viable bone to hold the screws. This is the awful situation that this patient found herself in just a few months ago.
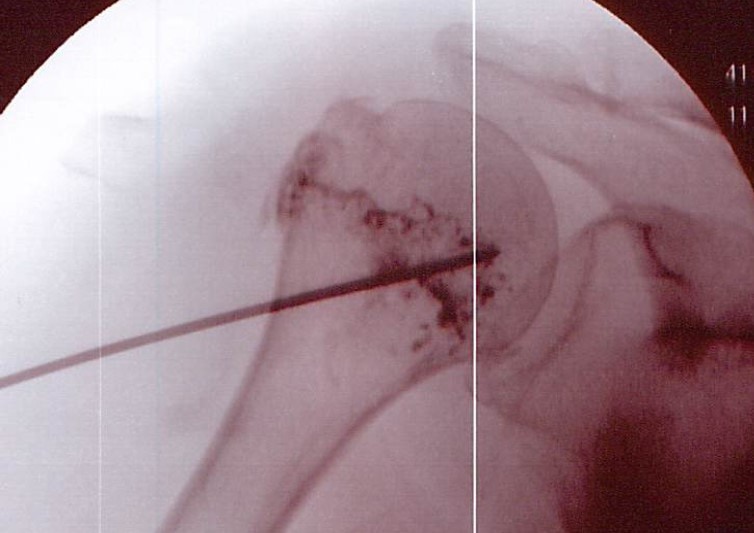
When Dr. Schultz first showed me this patient’s MRI, I think I sort of gasped and said, “Yikes”. We really didn’t know what would happen if we used precise imaging guidance to get her own highly concentrated stem cells (Regenexx-SD Procedure) into her fracture line using a stiff needle (trocar). However, she had no other options, so we were her last hope. Hence, below is the image of the trocar placed precisely into the fracture, with the dark contrast showing that the stem cells will go directly into the gap created by fracture.
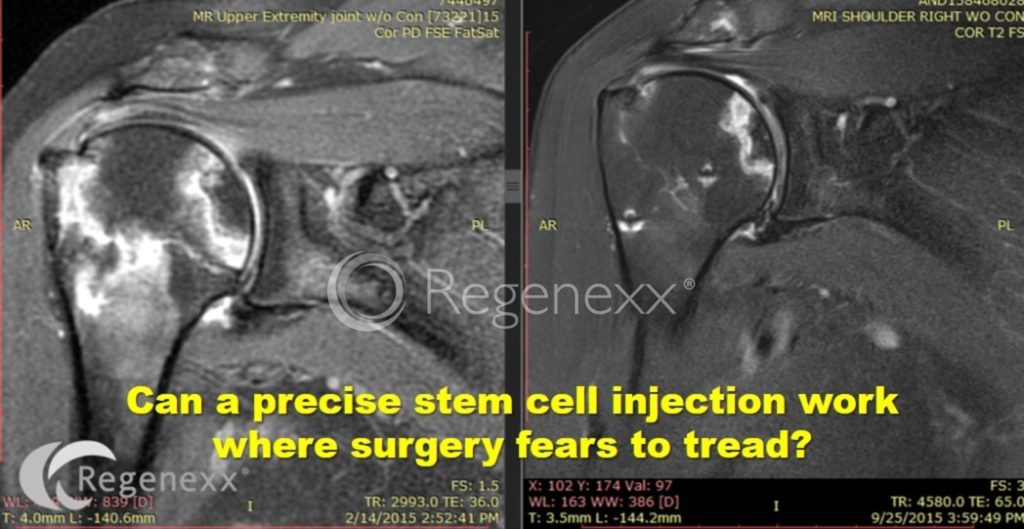
This patient’s before and after images are above. The white color in the humerus is all a serious problem, as it represents dead and fractured bone that won’t heal. You can see from the after picture on the right, that most of that white area is gone, now replaced with mostly healthy looking bone. The biggest problem spot that remains is the osteonecrosis area closer to the shoulder joint. You can see by the contrast spread in the fluoroscopy image above that this is an area that the stem cells didn’t reach. As a result, this is a patient who will likely need a second shoulder stem cell injection to get into that AVN area under precise x-ray guidance.
The upshot? This woman now has a fighting chance of saving her shoulder due to precise interventional orthopedics using her own super concentrated stem cells. This is pretty amazing, given that she had almost zero chance of a surgery helping her shoulder. What other amazing things will precisely placed needles and orthobiologics be able to accomplish in the future that orthopedic surgery can’t?

If you have questions or comments about this blog post, please email us at [email protected]
NOTE: This blog post provides general information to help the reader better understand regenerative medicine, musculoskeletal health, and related subjects. All content provided in this blog, website, or any linked materials, including text, graphics, images, patient profiles, outcomes, and information, are not intended and should not be considered or used as a substitute for medical advice, diagnosis, or treatment. Please always consult with a professional and certified healthcare provider to discuss if a treatment is right for you.